Hip Pain
 Hip pain is a descriptive term for pain that is located around the hip joint region.
Hip pain is a descriptive term for pain that is located around the hip joint region.
Definition:
Hip pain is a descriptive term for pain that is located around the hip joint region. The hip joints attach the lower limbs to the trunk and hence, our body weight can be transferred downwards through the hip joints to the foot on the ground. The hip joint also provides motion in all 3 anatomical planes (flexion and extension in the sagittal plane, abduction and abduction in the coronal plane and internal and external rotation in the horizontal plane). Its range of motion is the second largest in the body, only to the shoulder joint.
Anatomy:
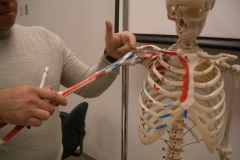
The hip joint is formed by the articulation of the rounded head of the femur and the cup-like acetabulum of the pelvis. The joint surfaces on either side are covered with a strong but lubricated layer of hyaline cartilage. The articulation is covered by the joint capsule which, in turn, is reinforced by surrounding ligaments to provide mobility, stability and to prevent excessive movements of the joint.
There are 4 extra-capsular ligaments. The three strong ligaments are iliofemoral, ischiofemoral, and pubofemoral ligaments, which attach to the corresponding part of the pelvis, the ilium, the ischium and the pubic bone on one end and to the femoral bone on the other end. The Y-shaped and twisted iliofemoral ligament is the strongest ligament in the human body. In standing position, it prevents our body from falling backward without the need of muscular activity. The ischiofemoral ligament prevents excessive medial rotation while the pubofemoral ligament restricts excessive abduction in the hip joint. The fourth ligament is zona orbicularis, which is a collar ring ligament around the narrowest part of the femoral neck at the base of the head of femur. It is formed by the circular fibers of the articular capsule of the hip joint and acts like a buttonhole on the femoral head to maintain its contact with the acetabulum fossa.
Hip pathologies:
The pathologies of hip joint can be classified according to the cause:
It is interesting that hip joint problems are not uncommon in the paediatric patient group. Transient synovitis which may be caused by viral infection is a common cause of hip pain and limping gait in children. Perthes disease is a temporary loss of blood supply to the femoral head among children which can lead to avascular necrosis of the head of femur if left untreated. It is much more common in boys than girls (4:1). Slipped capital femoral epiphysis occurs less commonly, but can affect children and adolescents with boys to girls about 2:1. It is caused by the displacement of the femoral head along the unstable growth plate posteriorly and inferiorly in relation to the femoral neck and within the confines of the acetabulum. In general, about 20% of patients have bilateral involvement at the time of presentation. There is an increased risk in children who are obese moves through the growth plate relative to the rest of femur.
Symptoms and signs:
The symptoms and signs are variable depending on the underlying pathology. Hip pain can be caused by pathologies inside the hip, pain referred from other structures to the hip and pain generated biomechanically from problems of the back above and knee and foot below.
Hip-related pain is not always felt directly over the hip. As the hip joint is three-dimensional, pain may be also felt along the outside part of the hip, in the buttock area or even radiate down to the knee region.
Pain from other sources, like low back, sacroiliac joint, knee joints or even pelvic organs, can be referred to the hip. Iliopsoas strain or iliopsoas bursitis are two common causes of groin pain that can be mistaken as hip pain. Typically the pain is felt in the front of the hip and groin and is aggravated by flexion of the hip – as with going up stairs. It is crucial to look for other primary pathology if hip joint examination is unremarkable. Among the other common causes are adductor strain or adductor tendinitis (groin pull) which are most common in sprinters. Occasionally, pain around the hip can be referred pain from trigger points of the Quadratus lumborum muscle.
Pain in the hip can be generated from overuse use or misuse of the hip because of biomechanical derangements. Abnormal gait can cause pain inside the hip. Limping can be caused by problems in the foot, ankle and knee. It is the way that our body compensates for pain by trying to reduce the force loaded onto the joint with pathology while walking. Limping is never normal. When limping occurs, abnormal stresses are placed on the joints above and below. In the case of knee problems, for example, the body loading will be shifted upward to the hip and downward to ankle causing hip and ankle pain.
Reduced range of movement can be found if the joint is degenerated or acutely inflamed. The most commonly affected movement is internal rotation of the hip joint. Rarely, swelling and erythema can be found around an inflamed hip joint as the joint is deeply located.
Investigations:
Hip pain is a non-specific complaint that requires a doctor to work out the exact underlying causes. Therefore, careful history and physical examination are important. Investigations are sometimes needed to confirm the diagnosis. X-ray hip is a simple and safe procedure to document fracture, dislocation and late avascular necrosis of the hip. Musculoskeletal ultrasound can helps to visual tendinosis, muscle tear and inflamed bursitis. CT scan can help to pick up some subtle fracture. MRI is good to see surrounding soft tissue, but expensive. A musculoskeletal physician will have the expertise to diagnosis a hip pain and confirm the diagnosis, if necessary, with the most cost-effective investigation.
Treatment:
Treatment depends on the cause of hip pain. For hip OA, a musculoskeletal physician will use non surgical treatments like weight reduction, analgesics and physical therapy. For those severe cases that do not respond well, prolotherapy is employed to strengthen the degenerated hip ligaments and stabilize the hip joint to reduce pain. Prolotherapy is especially good for those patients who do not opt for total hip replacement surgery. Surgery is the best treatment method for fracture neck of femur. Immunotherapy is an advanced treatment for hip pain from autoimmune diseases.
髖痛症
 髖痛症是一個描述髖部疼痛的名詞
髖痛症是一個描述髖部疼痛的名詞
定義:
是一個描述髖部疼痛的名詞。髖關節連接下肢與軀幹,所以體重可通過髖關節向下傳遞至雙足。髖關節可進行3個解剖平面的活動(矢狀面的屈、伸;冠狀面的內收、外展;以及水平面的內旋、外旋),活動範圍之廣佔人體關節中的第二大,僅次於肩關節。
解剖學:
髖關節是由圓形的股骨頭和杯狀的髖臼形成。整個關節面均有強健而又潤滑的透明軟骨覆蓋。關節外被關節囊及囊外韌帶包蓋,令關節的活動靈活而穩定並防止過度活動。
髖關節有4條囊外韌帶,其中三條較堅韌的是髂股、坐股、恥股韌帶,一端附著於骨盆的相應部位,即髂骨、坐骨、恥骨,另一端附著於股骨。Y字形並向前旋走的髂股韌帶是人體中最堅韌的韌帶,它在無需肌肉收縮的情況下仍可防止人體於站立時向後傾倒。坐股韌帶可防止髖關節過度內旋,而恥股韌帶防止過度外展。第四組韌帶是輪匝帶,由髖關節囊的環狀纖維形成,呈項圈狀圍繞在股骨頭基底,股骨頸最窄的部分,有鈕扣孔樣作用使股骨頭與髖臼保持連接。
病理學:
髖關節的病變按病因分為:
小童的髖關節問題並不少見。病毒感染引起的暫時性滑膜炎 (transient synovitis) 是小童髖關節痛和跛行的常見原因。Perthes 病是由於股骨頭的血液供應暫時受阻所致,若不給予治療會發展為缺血性壞死,男孩發病遠多於女孩(4:1)。股骨頭骨骺滑脫症較少見,但偶爾也會發生於兒童和青少年,是由於股骨頭在髖臼內沿未癒合的骺板向後和向下移位造成,總體來講,男女比例為 2:1,就診時雙側受累者佔 20%,肥胖兒童發病風險增高。
症狀與表徵:
症狀和表徵隨不同病因而不同。髖痛可由髖部病變引起,髖痛也可由其他部位放射至髖部,也可因背部、膝部或足部等生物力學改變所引起。
與髖關節相關的疼痛並非只局限於關節內。因為髖關節是一個三維活動的關節,所以疼痛可處於髖部外側及臀部,甚至疼痛可放射至膝部。
一些其他部位如,腰背部、骶髂關節、膝關節甚至盆腔器官的疼痛可放射至髖部。髖痛症若檢查髖關節無異常發現,則應尋找其他原發病變。髂腰肌勞損或髂腰肌滑囊炎是引起腹股溝痛的兩個常見原因,可與髖痛症混淆,其典型的痛處是在髖關節和腹股溝前面,而且屈髖時,例如上樓梯,疼痛會加重。其他原發病變如內收肌勞損或內收肌腱炎也較常見,這兩種情況多見於賽跑選手。髖部的疼痛偶爾也可以是腰方肌激痛點產生的轉移痛。
髖痛症的疼痛還可來自因髖部過度或非正常使用所產生的生物力學紊亂所引致。不正常步態可引起髖痛症。足、踝和膝的病變可導致跛行,跛行是絕對不正常的。跛行其實是身體對痛楚的代償機制,因行走時盡量減少在患處所負的體重,導致不正常的應力轉移到患處的上位和下位關節。比如,膝關節問題時,身體的負重會轉移至上位的髖部及下位的踝部而導致髖痛和踝痛。
髖部活動範圍受限可見於退化性或急性髖關節炎,關節活動受影響最大的是內旋。
因為髖關節位置深,所以很少見到紅腫的髖關節炎。
實驗室檢查:
髖痛是一種非特異性的症狀,所以需要醫生找出確切的病因。因此詳細的病史和臨床檢查非常重要。有時也需要實驗室檢查來確定診斷。X光是診斷髖部骨折、脫臼和晚期缺血性壞死簡單而安全的方法。肌骼超聲波有助於肌腱病、肌束撕裂和滑囊炎的診斷。電腦掃描有助於不明顯骨折的診斷。MRI是觀察關節週圍軟組織的理想方法,但卻昂貴。肌骼科醫生應用專業知識來診斷髖痛症,在考慮成本效益的情況下,建議採用某些檢查確定診斷。
治療:
治療方法取決於髖痛症的病因。對於髖關節退化性骨關節炎,肌骼科醫生會用非手術的方法治療,如,減肥、止痛和物理治療。病情嚴重而且對上述治療反應不良時,可用保絡治療強化退變的韌帶,使髖骨節穩定並減輕疼痛。保絡治療尤其對不願接受全髖關節置換術的患者尤為理想。手術是治療股骨頸骨折的最佳選擇。免疫療法是新的治療方法,用於免疫性疾病所致的髖痛。